-
 Rtf1 Transcriptionally Regulates Neonatal and Adult Cardiomyocyte Biology
Rtf1 Transcriptionally Regulates Neonatal and Adult Cardiomyocyte Biology -
 Left Atrial Strain Imaging by Speckle Tracking Echocardiography: The Supportive Diagnostic Value in Cardiac Amyloidosis and Hypertrophic Cardiomyopathy
Left Atrial Strain Imaging by Speckle Tracking Echocardiography: The Supportive Diagnostic Value in Cardiac Amyloidosis and Hypertrophic Cardiomyopathy -
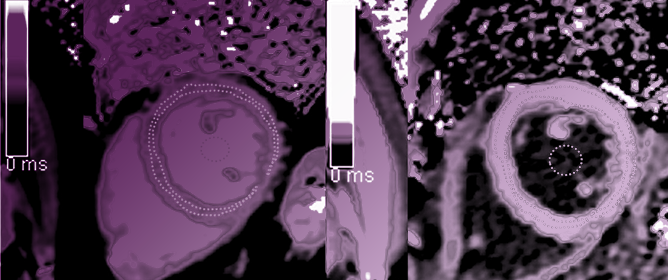 Longitudinal Changes in the Myocardial T1 Relaxation Time, Extracellular Volume Fraction, and Left Ventricular Function in Asymptomatic Men
Longitudinal Changes in the Myocardial T1 Relaxation Time, Extracellular Volume Fraction, and Left Ventricular Function in Asymptomatic Men -
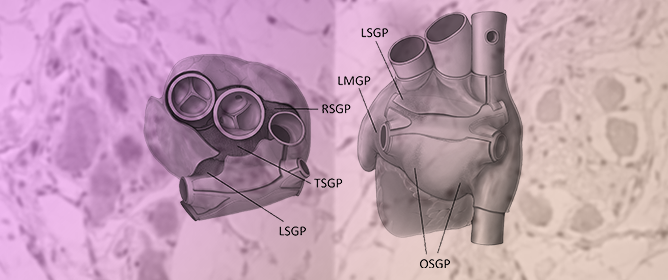 Cardioneuroablation Using Epicardial Pulsed Field Ablation for the Treatment of Atrial Fibrillation
Cardioneuroablation Using Epicardial Pulsed Field Ablation for the Treatment of Atrial Fibrillation
Journal Description
Journal of Cardiovascular Development and Disease
Journal of Cardiovascular Development and Disease
is an international, scientific, peer-reviewed, open access journal on cardiovascular medicine published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: CiteScore - Q2 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.1 days after submission; acceptance to publication is undertaken in 2.5 days (median values for papers published in this journal in the first half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.4 (2022);
5-Year Impact Factor:
3.0 (2022)
Latest Articles
The Effect of Daylight-Saving Time on Percutaneous Coronary Intervention Outcomes in Acute Coronary Syndrome Patients—Data from the Polish National Registry of Percutaneous Coronary Interventions (ORPKI) in the Years 2014–2022
J. Cardiovasc. Dev. Dis. 2023, 10(9), 375; https://doi.org/10.3390/jcdd10090375 (registering DOI) - 01 Sep 2023
Abstract
►
Show Figures
Introduction: Many factors related to the switch to summer/winter time interfere with biological rhythms. Objectives: This study aimed to analyze the impact of time change on clinical outcomes of patients with acute coronary syndromes (ACS) undergoing percutaneous coronary intervention (PCI). Patients and methods:
[...] Read more.
Introduction: Many factors related to the switch to summer/winter time interfere with biological rhythms. Objectives: This study aimed to analyze the impact of time change on clinical outcomes of patients with acute coronary syndromes (ACS) undergoing percutaneous coronary intervention (PCI). Patients and methods: Electronic data of 874,031 patients with ACS who underwent invasive procedures were collected from the Polish National Register of Interventional Cardiology Procedures (ORPKI) between 2014 and 2021. We determined the number of patients undergoing PCI and periprocedural mortality during the day of spring or autumn time change and within the first 3 and 7 days after the time change. Results: We demonstrated the impact of time changes on the periprocedural mortality of ACS patients within 1 day and the period of 3 and 7 days from the time change. We observed that the occurrence of all ACS and NSTEMI on the first day was lower for both time changes and higher in the case of UA and spring time change. The autumn time change significantly reduced the occurrence of all types of ACS. A significant decrease in the number of invasive procedures was found after autumn transition in the period from the first day to 7 days for ACS, NSTEMI, and UA. Conclusions: The occurrence of ACS and the number of invasive procedures were lower for both changes over time. Autumn time change is associated with increased periprocedural mortality in ACS and a less frequent occurrence of UA and NSTEMI within 7 days.
Full article
Open AccessCase Report
ST-Segment Elevation: An Unexpected Culprit
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 374; https://doi.org/10.3390/jcdd10090374 (registering DOI) - 01 Sep 2023
Abstract
The clinical presentation of pulmonary embolism (PE) and acute coronary syndrome can be similar. We report a case of a patient presenting with antero-septal ST-segment elevation after cardiac arrest, found to have acute-PE-mimicking ST-segment elevation myocardial infarction (STEMI), treated with aspiration thrombectomy and
[...] Read more.
The clinical presentation of pulmonary embolism (PE) and acute coronary syndrome can be similar. We report a case of a patient presenting with antero-septal ST-segment elevation after cardiac arrest, found to have acute-PE-mimicking ST-segment elevation myocardial infarction (STEMI), treated with aspiration thrombectomy and catheter-directed thrombolysis (CDT). A 78-year-old man was admitted with dyspnea, chest pain and tachycardia. During evaluation, cardiac arrest in pulseless electrical activity was documented. Advanced life support was started immediately. ECG post-ROSC revealed ST-segment elevation in V1–V4 and aVR. Echocardiography showed normal left ventricular function but right ventricular (RV) dilation and severe dysfunction. The patient was in shock and was promptly referred to cardiac catheterization that excluded significant CAD. Due to the discordant ECG and echocardiogram findings, acute PE was suspected, and immediate invasive pulmonary angiography revealed bilateral massive pulmonary embolism. Successful aspiration thrombectomy was performed followed by local alteplase infusion. At the end of the procedure, mPAP was reduced and blood pressure normalized allowing withdrawal of vasopressor support. Twenty-four-hour echocardiographic reassessment showed normal-sized cardiac chambers with preserved biventricular systolic function. Bedside echocardiography in patients with ST-segment elevation post-ROSC is instrumental in raising the suspicion of acute PE. In the absence of a culprit coronary lesion, prompt pulmonary angiography should be considered if immediately feasible. In these cases, CDT and aspiration in high-risk acute PE seem safe and effective in relieving obstructive shock and restoring hemodynamics.
Full article
(This article belongs to the Section Acquired Cardiovascular Disease)
►▼
Show Figures

Figure 1
Open AccessReview
Prosthesis–Patient Mismatch and Aortic Root Enlargement: Indications, Techniques and Outcomes
by
and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 373; https://doi.org/10.3390/jcdd10090373 (registering DOI) - 01 Sep 2023
Abstract
Prosthesis–patient mismatch (PPM) is defined as implanting a prosthetic that is insufficiently sized for the patient receiving it. PPM leads to high residual transvalvular gradients post-aortic valve replacement and consequently results in left ventricular dysfunction, morbidity and mortality in both the short and
[...] Read more.
Prosthesis–patient mismatch (PPM) is defined as implanting a prosthetic that is insufficiently sized for the patient receiving it. PPM leads to high residual transvalvular gradients post-aortic valve replacement and consequently results in left ventricular dysfunction, morbidity and mortality in both the short and long term. Younger patients and patients with poor preoperative left ventricular function are more vulnerable to increased mortality secondary to PPM. There is debate over the measurement of valvular effective orifice area (EOA) and variation exists in how manufacturers report the EOA. The most reliable technique is using in vivo echocardiographic measurements to create tables of predicted EOAs for different valve sizes. PPM can be prevented surgically in patients at risk through aortic root enlargement (ARE). Established techniques include the posterior enlargement through Nicks and Manouguian procedures, and aortico-ventriculoplasty with the Konno–Rastan procedure, which allows for a greater enlargement but carries increased surgical risk. A contemporary development is the Yang procedure, which uses a Y-shaped incision created through the non- and left-coronary cusp commissure, undermining the nadirs of the non- and left-coronary cusps. Early results are promising and demonstrate an ability to safely increase the aortic root by up to two to three sizes. Aortic root enlargement thus remains a valuable and safe tool in addressing PPM, and should be considered during surgical planning.
Full article
(This article belongs to the Special Issue Contemporary Clinical Treatment Options and Outcomes of Aortic Valve Disease)
►▼
Show Figures
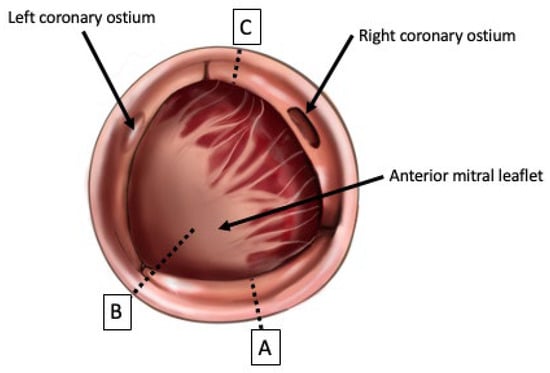
Figure 1
Open AccessArticle
Aortic Valve Dysfunction and Aortopathy Based on the Presence of Raphe in Patients with Bicuspid Aortic Valve Disease
J. Cardiovasc. Dev. Dis. 2023, 10(9), 372; https://doi.org/10.3390/jcdd10090372 - 31 Aug 2023
Abstract
(1) Background: To identify the association between the presence or absence of a raphe and aortic valve dysfunction, as well as the presence of aortopathy in patients with a bicuspid aortic valve (BAV); (2) Methods: This retrospective study enrolled 312 participants (mean (SD)
[...] Read more.
(1) Background: To identify the association between the presence or absence of a raphe and aortic valve dysfunction, as well as the presence of aortopathy in patients with a bicuspid aortic valve (BAV); (2) Methods: This retrospective study enrolled 312 participants (mean (SD) age, 52.7 (14.3) years; 227 men (72.8%)) with BAV. The BAVs were divided into those with the presence (raphe+) or absence (raphe−) of a raphe. Valvular function was classified as normal, aortic regurgitation (AR), or aortic stenosis (AS) using TTE. The pattern of BAV aortopathy was determined by the presence of dilatation at the sinus of Valsalva and the middle ascending aorta using CCT; (3) Results: BAVs with raphe+ had a higher prevalence of AR (148 (79.5%) vs. 48 (37.8%), p < 0.001), but a lower prevalence of AS (90 (48.6%) vs. 99 (78.0%), p < 0.001) compared with those with raphe−. The types of BAV aortopathy were significantly different (p = 0.021) according to those with BAV–raphe+ and BAV–raphe−; (4) Conclusions: The presence of a raphe was significantly associated with a higher prevalence of AR, but a lower prevalence of AS and combined dilatation of the aortic root and middle ascending aorta. The presence of a raphe was an independent determinant of AR.
Full article
(This article belongs to the Special Issue Current Practice in Cardiac Imaging)
►▼
Show Figures
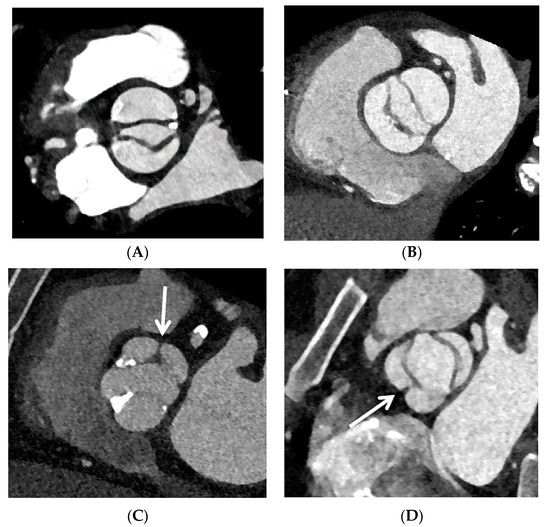
Figure 1
Open AccessReview
Anatomic Variations of Renal Arteries as an Important Factor in the Effectiveness of Renal Denervation in Resistant Hypertension
by
, , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 371; https://doi.org/10.3390/jcdd10090371 - 29 Aug 2023
Abstract
Hypertension remains the leading cause of death worldwide. Despite advances in drug-based treatment, many patients do not achieve target blood pressure. In recent years, there has been an increased interest in invasive hypertension treatment methods. Long-term effects and factors affecting renal denervation effectiveness
[...] Read more.
Hypertension remains the leading cause of death worldwide. Despite advances in drug-based treatment, many patients do not achieve target blood pressure. In recent years, there has been an increased interest in invasive hypertension treatment methods. Long-term effects and factors affecting renal denervation effectiveness are still under investigation. Some investigators found that the renal arteries’ morphology is crucial in renal denervation effectiveness. Accessory renal arteries occur in 20–30% of the population and even more frequently in patients with resistant hypertension. Diversity in renal vascularization and innervation may complicate the renal denervation procedure and increase the number of people who will not benefit from treatment. Based on previous studies, it has been shown that the presence of accessory renal arteries, and in particular, the lack of their complete denervation, reduces the procedure’s effectiveness. The following review presents the anatomical assessment of the renal arteries, emphasizing the importance of imaging tests. Examples of imaging and denervation methods to optimize the procedure are presented. The development of new-generation catheters and the advancement in knowledge of renal arteries anatomy may improve the effectiveness of treatment and reduce the number of patients who do not respond to treatment.
Full article
(This article belongs to the Section Imaging)
►▼
Show Figures
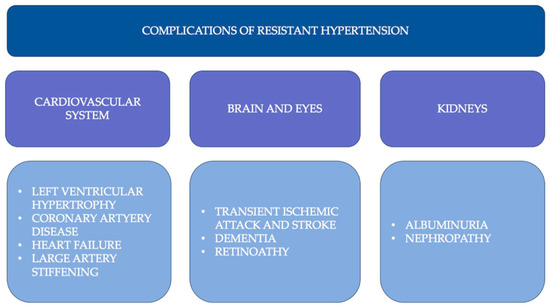
Figure 1
Open AccessCase Report
Cor Triatriatum Dexter Associated with an Ostium Primum Atrial Defect and Left-Sided Opening of the Coronary Sinus in a Stillborn Fetus
by
, , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 370; https://doi.org/10.3390/jcdd10090370 - 28 Aug 2023
Abstract
Cor triatriatum is a very rare cardiac malformation characterized by the presence of an abnormal interatrial membrane separating either the left or right atrial chamber into two compartments. It can be associated with other cardiac defects and is often symptomatic in childhood. The
[...] Read more.
Cor triatriatum is a very rare cardiac malformation characterized by the presence of an abnormal interatrial membrane separating either the left or right atrial chamber into two compartments. It can be associated with other cardiac defects and is often symptomatic in childhood. The signs depend on the size and position of the interatrial membrane and other associated malformations. Here we report a case of right-sided cor triatriatum associated with an ostium primum-type interatrial septum defect and left-sided opening of the coronary sinus in a fetus. The cause of intrauterine death was asphyxia due to total placental abruption.
Full article
(This article belongs to the Section Pediatric Cardiology and Congenital Heart Disease)
►▼
Show Figures
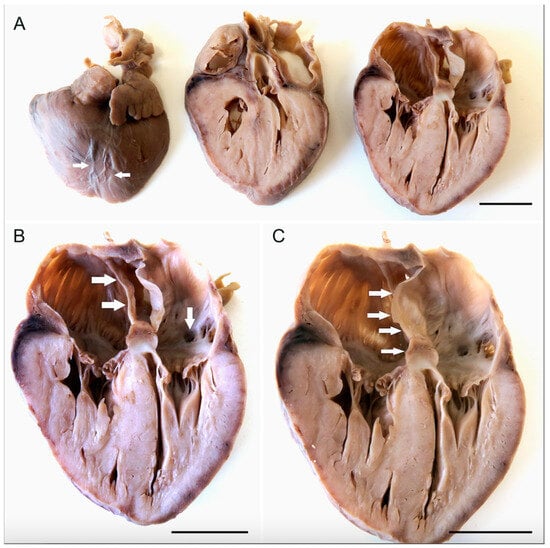
Figure 1
Open AccessArticle
Long-Term Prognosis of Different Subtypes of Left Ventricular Noncompaction Cardiomyopathy Patients: A Retrospective Study in China
by
, , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 369; https://doi.org/10.3390/jcdd10090369 - 28 Aug 2023
Abstract
Left ventricular noncompaction (LVNC) is a heterogeneous cardiomyopathy that can be classified into different subtypes based on morphologic and functional features. However, the prognosis of the dilated and isolated subtypes of non-pediatric LVNC remains unknown. We retrospectively studied 101 patients with LVNC diagnosed
[...] Read more.
Left ventricular noncompaction (LVNC) is a heterogeneous cardiomyopathy that can be classified into different subtypes based on morphologic and functional features. However, the prognosis of the dilated and isolated subtypes of non-pediatric LVNC remains unknown. We retrospectively studied 101 patients with LVNC diagnosed at Peking Union Medical College Hospital from 2006 to 2022 using the Jenni criteria of transthoracic echocardiography. The patients were grouped into those with dilated LVNC (n = 64) or isolated LVNC (n = 37), and 88 patients (54 with dilated LVNC and 34 with isolated LVNC) were followed up successfully. The primary outcome was major adverse cardiovascular events (a composite of cardiovascular mortality, heart failure, severe ventricular arrhythmia, and systolic embolism). The median follow-up time was 5.24 years. The incidence of major adverse cardiovascular events was 43.2%; patients with dilated LVNC had a higher risk (adjusted hazard ratio, 4.43; 95% confidence interval, 1.24–15.81; p = 0.02) than those with isolated LVNC. None of the isolated LVNC patients had cardiovascular deaths or severe ventricular arrhythmias. The risk of systemic embolism was similar between patients with dilated and isolated LVNC. Our findings indicate that transthoracic echocardiography is a useful tool for classifying LVNC into subtypes with distinct clinical outcomes. Dilated LVNC is associated with a poor prognosis, while the isolated subtype is probably a physiological condition.
Full article
(This article belongs to the Special Issue Risk Factors, Diagnosis, and Treatment of Cardiovascular Disease)
►▼
Show Figures

Figure 1
Open AccessArticle
Prevalence, Risk Factors, Prognosis, and Management of Pericardial Effusion in COVID-19
by
, , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 368; https://doi.org/10.3390/jcdd10090368 - 27 Aug 2023
Abstract
Background: There is limited data in the literature about the clinical importance and prognosis of pericardial effusion (PE) in patients discharged after recovering from COVID-19, but large-scale studies have yet to be available. This study investigated the prevalence, risk factors, prognosis, late clinical
[...] Read more.
Background: There is limited data in the literature about the clinical importance and prognosis of pericardial effusion (PE) in patients discharged after recovering from COVID-19, but large-scale studies have yet to be available. This study investigated the prevalence, risk factors, prognosis, late clinical outcomes, and management of PE in COVID-19. Materials and Methods: Between August 2020 and March 2021, 15,689 patients were followed up in our pandemic hospital due to COVID-19. Patients with positive polymerase chain reaction (PCR) test results and PE associated with COVID-19 in computed tomography (CT) were included in the study. The patients were divided into three groups according to PE size (mild, moderate, and large). Transthoracic echocardiography (TTE) records, laboratory data, clinical outcomes, and medical treatments of patients discharged from the hospital were retrospectively reviewed. Results: According to the PE size (mild, moderate, large) of 256 patients with PE at admission or discharge, the mean age was 62.17 ± 16.34, 69.12 ± 12.52, and 72.44 ± 15.26, respectively. The mean follow-up period of the patients was 25.2 ± 5.12 months. Of the patients in the study population, 53.5% were in the mild group, 30.4% in the moderate group, and 16.1% in the large group. PE became chronic in a total of 178 (69.6%) patients at the end of the mean three months, and chronicity increased as PE size increased. Despite the different anti-inflammatory treatments for PE in the acute phase, similar chronicity was observed. In addition, as the PE size increased, the patients’ frequency of hospitalization, complications, and mortality rates showed statistical significance between the groups. Conclusions: The clinical prognosis of patients presenting with PE was quite poor; as PE in size increased, cardiac and noncardiac events and mortality rates were significantly higher. Patients with large PE associated with COVID-19 at discharge should be monitored at close intervals due to the chronicity of PE and the increased risk of tamponade.
Full article
(This article belongs to the Special Issue Epidemiology and Risk of Cardiovascular Disease)
►▼
Show Figures
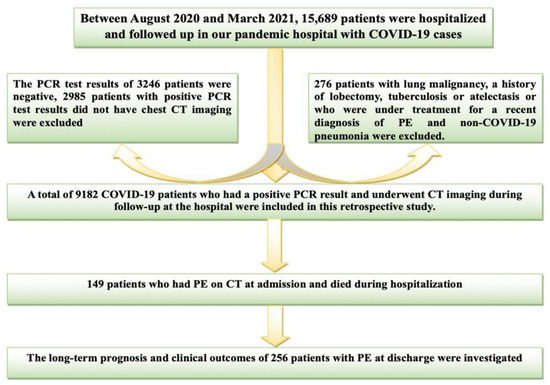
Figure 1
Open AccessArticle
Cardiac Morphology, Function, and Left Ventricular Geometric Pattern in Patients with Hypertensive Crisis: A Cardiovascular Magnetic Resonance-Based Study
J. Cardiovasc. Dev. Dis. 2023, 10(9), 367; https://doi.org/10.3390/jcdd10090367 - 27 Aug 2023
Abstract
(1) Background: Altered cardiac morphology and function are associated with increased risks of adverse cardiac events in hypertension. Our study aimed to assess left ventricular (LV) morphology, geometry, and function using cardiovascular magnetic resonance (CMR) imaging in patients with hypertensive crisis. (2) Methods:
[...] Read more.
(1) Background: Altered cardiac morphology and function are associated with increased risks of adverse cardiac events in hypertension. Our study aimed to assess left ventricular (LV) morphology, geometry, and function using cardiovascular magnetic resonance (CMR) imaging in patients with hypertensive crisis. (2) Methods: Patients with hypertensive crisis underwent CMR imaging at 1.5 Tesla to assess cardiac volume, mass, function, and contrasted study. Left ventricular (LV) function and geometry were defined according to the guideline recommendations. Late gadolinium enhancement (LGE) was qualitatively assessed and classified into ischemic and nonischemic patterns. Predictors of LGE was determined using regression analysis. (3) Results: Eighty-two patients with hypertensive crisis (aged 48.5 ± 13.4 years, and 57% males) underwent CMR imaging. Of these patients, seventy-eight percent were hypertensive emergency and twenty-two percent were urgency. Diastolic blood pressure was higher under hypertensive emergency (p = 0.032). Seventy-nine percent (92% of emergency vs. 59% of urgency, respectively; p = 0.003) had left ventricular hypertrophy (LVH). The most prevalent LV geometry was concentric hypertrophy (52%). Asymmetric LVH occurred in 13 (22%) of the participants after excluding ischemic LGE. Impaired systolic function occurred in 46% of patients, and predominantly involved hypertensive emergency. Nonischemic LGE occurred in 75% of contrasted studies (67.2% in emergency versus 44.4% in urgency, respectively; p < 0.001). Creatinine and LV mass were independently associated with nonischemic LGE. (5) Conclusion: LVH, altered geometry, asymmetric LVH, impaired LV systolic function, and LGE are common under hypertensive crisis. LVH and LGE more commonly occurred under hypertensive emergency. Longitudinal studies are required to determine the prognostic implications of asymmetric LVH and LGE in hypertensive crisis.
Full article
(This article belongs to the Section Imaging)
►▼
Show Figures
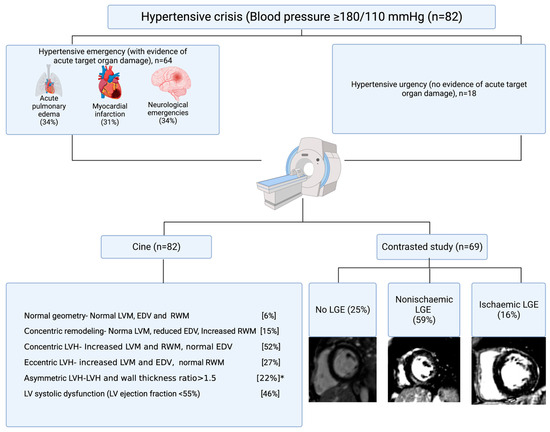
Figure 1
Open AccessArticle
Hemoadsorption Using CytoSorb® in Patients with Infective Endocarditis: A German-Based Budget Impact Analysis
by
, , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 366; https://doi.org/10.3390/jcdd10090366 - 26 Aug 2023
Abstract
A considerable number of infective endocarditis (IE) patients require cardiac surgery with an increased risk for postoperative sepsis. Intraoperative hemoadsorption may diminish the risk of postoperative hyperinflammation with potential economic implications for intensive care unit (ICU) occupation. The present study aimed to theoretically
[...] Read more.
A considerable number of infective endocarditis (IE) patients require cardiac surgery with an increased risk for postoperative sepsis. Intraoperative hemoadsorption may diminish the risk of postoperative hyperinflammation with potential economic implications for intensive care unit (ICU) occupation. The present study aimed to theoretically investigate the budget impact of a reduced length of ICU stay in IE patients treated with intraoperative hemoadsorption in the German healthcare system. Data on ICU occupation were extrapolated from a retrospective study on IE patients treated with hemoadsorption. An Excel-based budget impact model was developed to simulate the patient course over the ICU stay. A base-case scenario without therapy reimbursement and a scenario with full therapy reimbursement were explored. The annual eligible German IE patient population was derived from official German Diagnostic-Related Group (DRG) volume data. One-way deterministic sensitivity analysis and multivariate analysis were performed to evaluate the uncertainty over the model results. The use of intraoperative hemoadsorption resulted in EUR 2298 being saved per patient in the base-case scenario without therapy reimbursement. The savings increased to EUR 3804 per patient in the case of full device-specific reimbursement. Deterministic and probabilistic sensitivity analyses confirmed the robustness of savings, with a probability of savings of 87% and 99% in the base-case and full reimbursement scenario, respectively. Intraoperative hemoadsorption in IE patients might have relevant economic benefits related to reduced ICU stays, resulting in improved resource use. Further evaluations in larger prospective cohorts are warranted.
Full article
(This article belongs to the Special Issue Two of the Current Hot Challenges in Cardiac Surgery: Rising Endocarditis Cases and Extensive Use of Antithrombotics)
►▼
Show Figures
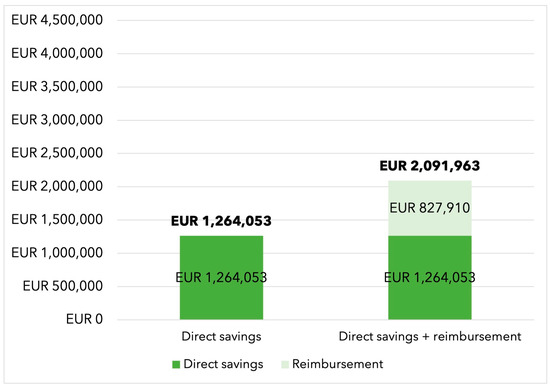
Figure 1
Open AccessArticle
Non-Invasive Risk Assessment and Prediction of Mortality in Patients Undergoing Coronary Artery Bypass Graft Surgery
by
, , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 365; https://doi.org/10.3390/jcdd10090365 - 25 Aug 2023
Abstract
Objectives: Heart rate turbulence (HRT) and T-wave alternans (TWA), non-invasive markers of cardiac autonomic dysfunction, and ventricular repolarization abnormality, reportedly, predict the risk of cardiovascular death after myocardial infarction. We investigated whether pre-operative assessment of HRT and/or TWA could predict long-term mortality following
[...] Read more.
Objectives: Heart rate turbulence (HRT) and T-wave alternans (TWA), non-invasive markers of cardiac autonomic dysfunction, and ventricular repolarization abnormality, reportedly, predict the risk of cardiovascular death after myocardial infarction. We investigated whether pre-operative assessment of HRT and/or TWA could predict long-term mortality following coronary artery bypass graft (CABG) surgery. Methods: From May 2010 to December 2017, patients undergoing elective CABG and receiving 24 h ambulatory electrocardiogram monitoring 1 to 5 days prior to CABG surgery were prospectively enrolled. Pre-operative HRT and TWA were measured using a 24 h ambulatory electrocardiogram. The relative risk of cardiac or overall death was assessed according to abnormalities of HRT, TWA, or left ventricular ejection fraction (LV EF). Results: During the mean follow-up period of 4.6
(This article belongs to the Special Issue Arrhythmic Risk Stratification)
►▼
Show Figures
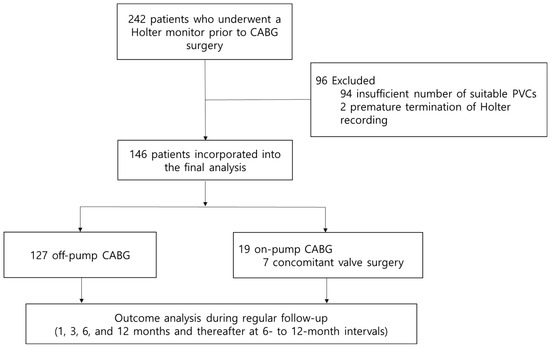
Figure 1
Open AccessReview
Contemporary Evaluation and Clinical Treatment Options for Aortic Regurgitation
J. Cardiovasc. Dev. Dis. 2023, 10(9), 364; https://doi.org/10.3390/jcdd10090364 - 25 Aug 2023
Abstract
Aortic regurgitation (AR) is the third most frequent form of valvular disease and has increasing prevalence with age. This will be of increasing clinical importance with the advancing age of populations around the globe. An understanding of the various etiologies and mechanisms leading
[...] Read more.
Aortic regurgitation (AR) is the third most frequent form of valvular disease and has increasing prevalence with age. This will be of increasing clinical importance with the advancing age of populations around the globe. An understanding of the various etiologies and mechanisms leading to AR requires a detailed understanding of the structure of the aortic valve and aortic root. While acute and chronic AR may share a similar etiology, their hemodynamic impact on the left ventricle (LV) and management are very different. Recent studies suggest current guideline recommendations for chronic disease may result in late intervention and suboptimal outcomes. Accurate quantitation of ventricular size and function, as well as grading of the severity of regurgitation, requires a multiparametric and multimodality imaging approach with an understanding of the strengths and weaknesses of each metric. Echocardiography remains the primary imaging modality for diagnosis with supplemental information provided by computed tomography (CT) and cardiac magnetic resonance imaging (CMR). Emerging transcatheter therapies may allow the treatment of patients at high risk for surgery, although novel methods to assess AR severity and its impact on LV size and function may improve the timing and outcomes of surgical intervention.
Full article
(This article belongs to the Special Issue Contemporary Clinical Treatment Options and Outcomes of Aortic Valve Disease)
►▼
Show Figures

Figure 1
Open AccessReview
Cardiovascular Applications of Photon-Counting CT Technology: A Revolutionary New Diagnostic Step
by
, , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 363; https://doi.org/10.3390/jcdd10090363 - 25 Aug 2023
Abstract
►▼
Show Figures
Photon-counting computed tomography (PCCT) is an emerging technology that can potentially transform clinical CT imaging. After a brief description of the PCCT technology, this review summarizes its main advantages over conventional CT: improved spatial resolution, improved signal and contrast behavior, reduced electronic noise
[...] Read more.
Photon-counting computed tomography (PCCT) is an emerging technology that can potentially transform clinical CT imaging. After a brief description of the PCCT technology, this review summarizes its main advantages over conventional CT: improved spatial resolution, improved signal and contrast behavior, reduced electronic noise and artifacts, decreased radiation dose, and multi-energy capability with improved material discrimination. Moreover, by providing an overview of the existing literature, this review highlights how the PCCT benefits have been harnessed to enhance and broaden the diagnostic capabilities of CT for cardiovascular applications, including the detection of coronary artery calcifications, evaluation of coronary plaque extent and composition, evaluation of coronary stents, and assessment of myocardial tissue characteristics and perfusion.
Full article
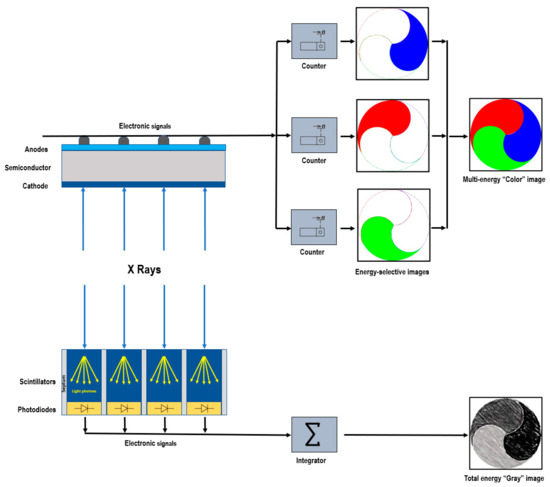
Figure 1
Open AccessArticle
Trends in Medical and Device Therapies Following Incident Heart Failure in Denmark during 1996–2019: A Nationwide Register-Based Follow-Up Study
by
, , , , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 362; https://doi.org/10.3390/jcdd10090362 - 25 Aug 2023
Abstract
Introduction: Data on temporal trends in guideline-based medical and device therapies in real-world chronic heart failure (HF) patients are lacking. Methods: Register-based nationwide follow-ups of temporal trends in characteristics, guideline-recommended therapies, one-year all-cause mortality, and HF rehospitalizations in incident HF patients in Denmark
[...] Read more.
Introduction: Data on temporal trends in guideline-based medical and device therapies in real-world chronic heart failure (HF) patients are lacking. Methods: Register-based nationwide follow-ups of temporal trends in characteristics, guideline-recommended therapies, one-year all-cause mortality, and HF rehospitalizations in incident HF patients in Denmark during 1996–2019. Results: Among 291,720 incident HF patients, the age at the onset of HF was stable over time. While initially fairly equal, the sex distribution markedly changed over time with more incidents occurring in men overall. Hypertension and diabetes increased significantly over time, while other comorbidities remained stable. Between 1996 and 2019, significant increases in angiotensin-converting enzyme inhibitor and angiotensin II-receptor blocker (ACEi/ARB) therapy (38.2% to 69.9%), beta-blocker therapy (15.5% to 70.6%), and mineralocorticoid receptor antagonist (MRA) therapy (11.8% to 34.5%) were seen. Angiotensin receptor-neprilysin inhibitor (ARNI) and sodium-glucose cotransporter-2 inhibitors (SGLT2i) were introduced in the middle of the past decade, with minor increases but overall low uses: ARNI (2015: 0.1% vs. 2019: 3.9%) and SGLT2i (2012: <0.1% vs. 2019: 3.9%). Between 1999 and 2019, implantable cardioverter-defibrillator (ICD) use increased significantly: 0.1% to 3–4%. Cardiac resynchronization therapy (CRT) use similarly increased between 2000 and 2019: 0.2% to 2.3%. Between 1996 and 2019, one-year all-cause mortality decreased significantly: 34.6% to 20.9%, as did HF rehospitalizations (6% to 1.3%). Conclusions: Among 291,720 incident HF patients in Denmark during 1996–2019, significant increases in the use of ACEi/ARB, beta-blockers, MRAs, and devices were seen, with concurrent significant decreases in the one-year all-cause mortality and HF rehospitalization rates. The use of CRT, ARNI, and SGLT2i remained low, and MRAs were relatively underutilized, thereby representing future targets to potentially further improve HF prognoses.
Full article
(This article belongs to the Special Issue Cardiovascular Disease Epidemiology: A Themed Issue in Honor of Dr. Alessandro Menotti on the Occasion of His 90th Birthday)
►▼
Show Figures

Figure 1
Open AccessReview
Myocardial Functional Imaging in Pediatric Nuclear Cardiology
by
, , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 361; https://doi.org/10.3390/jcdd10090361 - 24 Aug 2023
Abstract
The role of nuclear medicine in pediatric cardiology has grown rapidly over the years, providing useful functional and prognostic information and playing a complementary role to morphological imaging in the evaluation of myocardial perfusion, cardiovascular inflammation and infections, and cardiac sympathetic innervation. The
[...] Read more.
The role of nuclear medicine in pediatric cardiology has grown rapidly over the years, providing useful functional and prognostic information and playing a complementary role to morphological imaging in the evaluation of myocardial perfusion, cardiovascular inflammation and infections, and cardiac sympathetic innervation. The aim of this narrative review is to summarize and highlight the most important evidence on pediatric nuclear cardiology, describing clinical applications and the possibilities, advantages, and limitations of nuclear medicine techniques. Moreover, a special focus will be given to the minimization of radiation exposure in pediatric nuclear cardiology imaging, a critical topic in children.
Full article
(This article belongs to the Special Issue Advances in the Diagnosis of Cardiovascular Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Recognition of Supraventricular Arrhythmias in Holter ECG Recordings by ECHOView Color Map: A Case Series Study
J. Cardiovasc. Dev. Dis. 2023, 10(9), 360; https://doi.org/10.3390/jcdd10090360 - 24 Aug 2023
Abstract
Ambulatory 24–72 h Holter ECG monitoring is recommended for patients with suspected arrhythmias, which are often transitory and might remain unseen in resting standard 12-lead ECG. Holter manufacturers provide software diagnostic tools to assist clinicians in evaluating these large amounts of data. Nevertheless,
[...] Read more.
Ambulatory 24–72 h Holter ECG monitoring is recommended for patients with suspected arrhythmias, which are often transitory and might remain unseen in resting standard 12-lead ECG. Holter manufacturers provide software diagnostic tools to assist clinicians in evaluating these large amounts of data. Nevertheless, the identification of short arrhythmia events and differentiation of the arrhythmia type might be a problem in limited Holter ECG leads. This observational clinical study aims to explore a novel and weakly investigated ECG modality integrated into a commercial diagnostic tool ECHOView (medilog DARWIN 2, Schiller AG, Switzerland), while used for the interpretation of long-term Holter-ECG records by a cardiologist. The ECHOView transformation maps the beat waveform amplitude to a color-coded bar. One ECHOView page integrates stacked color bars of about 1740 sequential beats aligned by R-peak in a window (R ± 750 ms). The collected 3-lead Holter ECG recordings from 86 patients had a valid duration of 21 h 20 min (19 h 30 min–22 h 45 min), median (quartile range). The ECG rhythm was reviewed with 3491 (3192–3723) standard-grid ECG pages and a substantially few number of 51 (44–59) ECHOView pages that validated the ECHOView compression ratio of 67 (59–74) times. Comments on the ECG rhythm and ECHOView characteristic patterns are provided for 14 examples representative of the most common rhythm disorders seen in our population, including supraventricular arrhythmias (supraventricular extrasystoles, paroxysmal supraventricular arrhythmia, sinus tachycardia, supraventricular tachycardia, atrial fibrillation, and flutter) and ventricular arrhythmias (ventricular extrasystoles, non-sustained ventricular tachycardia). In summary, the ECHOView color map transforms the ECG modality into a novel diagnostic image of the patient’s rhythm that is comprehensively interpreted by a cardiologist. ECHOView has the potential to facilitate the manual overview of Holter ECG recordings, to visually identify short-term arrhythmia episodes, and to refine the diagnosis, especially in high-rate arrhythmias.
Full article
(This article belongs to the Special Issue Advanced Diagnostic Imaging for Cardiovascular Disease)
►▼
Show Figures
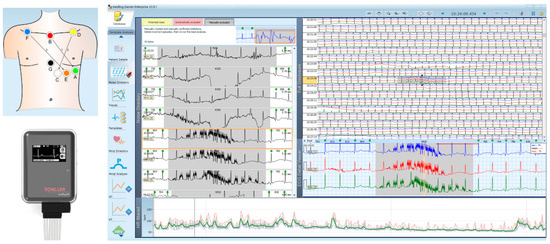
Figure 1
Open AccessArticle
Textural Analysis of the Hyperdense Artery Sign in Patients with Acute Ischemic Stroke Predicts the Outcome of Thrombectomy
by
, , , , , , , , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 359; https://doi.org/10.3390/jcdd10090359 - 24 Aug 2023
Abstract
Textural analysis is pivotal in augmenting the diagnosis and outcomes of endovascular procedures for stroke patients. Due to the detection of changes imperceptible to the human eye, this type of analysis can potentially aid in deciding the optimal type of endovascular treatment. We
[...] Read more.
Textural analysis is pivotal in augmenting the diagnosis and outcomes of endovascular procedures for stroke patients. Due to the detection of changes imperceptible to the human eye, this type of analysis can potentially aid in deciding the optimal type of endovascular treatment. We included 40 patients who suffered from acute ischemic stroke caused by large vessel occlusion, and calculated 130 different textural features based on the non-enhanced CT scan using an open-source software (3D Slicer). Using chi-squared and Mann–Whitney tests and receiver operating characteristics analysis, we identified a total of 21 different textural parameters capable of predicting the outcome of thrombectomy (quantified as the mTICI score), with variable sensitivity (50–97.9%) and specificity (64.6–99.4%) rates. In conclusion, CT-based radiomics features are potential factors that can predict the outcome of thrombectomy in patients suffering from acute ischemic stroke, aiding in the decision between aspiration, mechanical, or combined thrombectomy procedure.
Full article
(This article belongs to the Special Issue Stroke: Risk Factors, Mechanisms, Outcomes and Ethnicity)
►▼
Show Figures
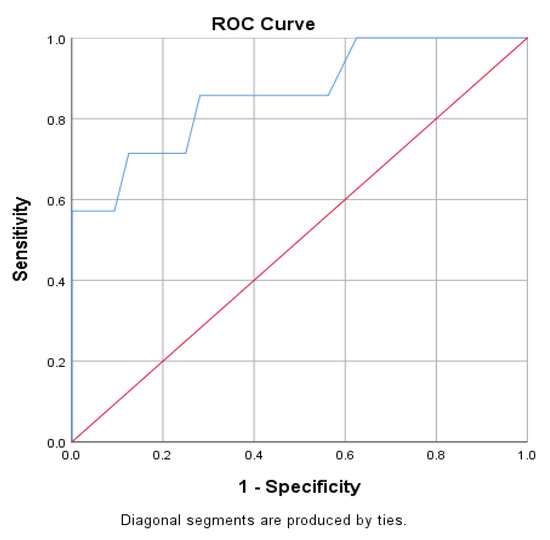
Figure 1
Open AccessArticle
The Association between Cardiovascular Risk Factors and Carotid Intima-Media Thickness in 42,726 Adults in UK Biobank: A Cross-Sectional Study
by
, , , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 358; https://doi.org/10.3390/jcdd10090358 - 23 Aug 2023
Abstract
►▼
Show Figures
Background: Traditional modifiable cardiovascular risk factors, such as high blood pressure, have long been positively correlated with high carotid intima-media thickness (cIMT). However, traditional cardiovascular risk factors made a minor contribution to cIMT variance, meaning that other markers may be regarded as independent
[...] Read more.
Background: Traditional modifiable cardiovascular risk factors, such as high blood pressure, have long been positively correlated with high carotid intima-media thickness (cIMT). However, traditional cardiovascular risk factors made a minor contribution to cIMT variance, meaning that other markers may be regarded as independent markers for increasing cIMT. Aims: To investigate the simple demographic patterns of carotid intima-media thickness (cIMT) in the UK Biobank and to identify which upstream cardiovascular disease (CVD) risk factors are independently associated with cIMT. Methods and Results: A cross-sectional-based study of healthy middle-aged people recruited in the UK between 2006 and 2010 (n = 42,726). Results: This study showed that the cardiovascular risk profile generally worsened across the cIMT quantiles from lowest to highest. The lowest cIMT quartile was defined as having a mean cIMT < 588 µm, while the highest cIMT quartile was defined as having a mean cIMT > 748 µm. Specifically, the highest cIMT quantile group had a worse CVD risk factors profile compared to the lowest cIMT quantile group. It was found that, for every one SD increase in age and systolic blood pressure, the mean cIMT increased by 0.357 SD and 0.115 SD, respectively. Conclusion: Systolic blood pressure and age were the strongest independent risk factors for a high cIMT value compared to other risk factors.
Full article
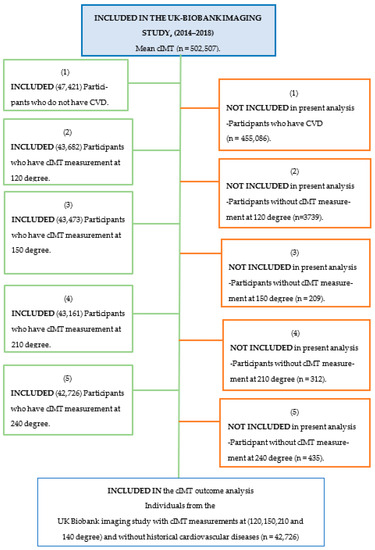
Figure 1
Open AccessReview
Comparative Analysis of Heart Regeneration: Searching for the Key to Heal the Heart—Part II: Molecular Mechanisms of Cardiac Regeneration
by
, , , and
J. Cardiovasc. Dev. Dis. 2023, 10(9), 357; https://doi.org/10.3390/jcdd10090357 - 22 Aug 2023
Abstract
Cardiovascular diseases are the leading cause of death worldwide, among which ischemic heart disease is the most representative. Myocardial infarction results from occlusion of a coronary artery, which leads to an insufficient blood supply to the myocardium. As it is well known, the
[...] Read more.
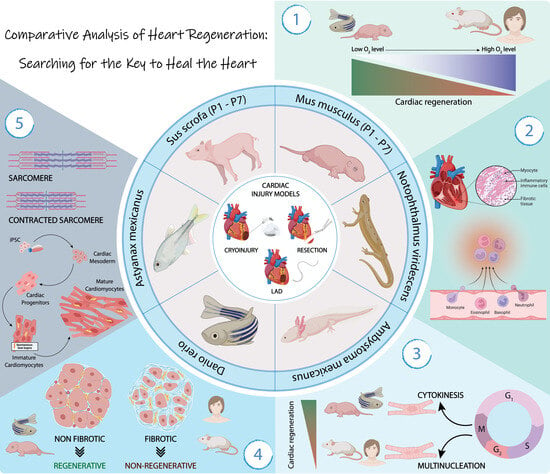
Cardiovascular diseases are the leading cause of death worldwide, among which ischemic heart disease is the most representative. Myocardial infarction results from occlusion of a coronary artery, which leads to an insufficient blood supply to the myocardium. As it is well known, the massive loss of cardiomyocytes cannot be solved due the limited regenerative ability of the adult mammalian hearts. In contrast, some lower vertebrate species can regenerate the heart after an injury; their study has disclosed some of the involved cell types, molecular mechanisms and signaling pathways during the regenerative process. In this ‘two parts’ review, we discuss the current state-of-the-art of the main response to achieve heart regeneration, where several processes are involved and essential for cardiac regeneration.
Full article
(This article belongs to the Special Issue Cardiac Development, Regeneration and Repair)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Early versus Delayed Surgery in Patients with Left-Sided Infective Endocarditis and Stroke
J. Cardiovasc. Dev. Dis. 2023, 10(8), 356; https://doi.org/10.3390/jcdd10080356 - 21 Aug 2023
Abstract
Background: Timing of surgery remains controversial in patients with infective endocarditis and stroke. Guidelines on infective endocarditis suggest delaying surgery for up to 4 weeks. However, with early heart failure due to progression of the infection or recurrent septic embolism, urgent surgery becomes
[...] Read more.
Background: Timing of surgery remains controversial in patients with infective endocarditis and stroke. Guidelines on infective endocarditis suggest delaying surgery for up to 4 weeks. However, with early heart failure due to progression of the infection or recurrent septic embolism, urgent surgery becomes imperative. Methods: Out of 688 patients who were surgically treated for left-sided infective endocarditis, 187 presented with preoperative neurological events. The date of cerebral stroke onset was documented in 147 patients. The patients were stratified according to timing of surgery: 61 in the early group (0–7 days) vs. 86 in the delayed group (>7 days). Postoperative neurological outcome was assessed by the modified Rankin Scale. Results: Preoperative sepsis was more prevalent in patients with preoperative neurological complications (46.0% vs. 29.5%, p < 0.001). Patients with haemorrhagic stroke were operated on later (19.8% vs. 3.3%, p = 0.003). Postoperative cerebrovascular accidents were comparable between both groups (p = 0.13). Overall, we observed good neurological outcomes (p = 0.80) and a high recovery rate, with only 5% of cases showing neurological deterioration after surgery (p = 0.29). In-hospital mortality and long-term survival were not significantly different in the early and delayed surgery groups (log-rank, p = 0.22). Conclusions: Early valve surgery in high-risk patients with infective endocarditis and stroke can be performed safely and is not associated with worse outcomes.
Full article
(This article belongs to the Special Issue Current Challenges in Heart Failure and Cardiac Transplantation)
►▼
Show Figures
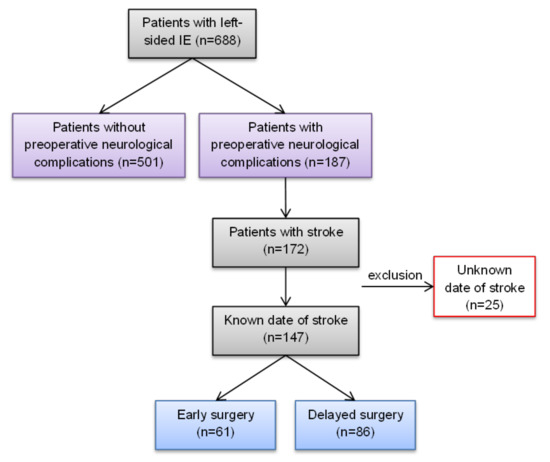
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Applied Biosciences, Bioengineering, Biomolecules, JCDD, JCM, Micromachines, Reports
Usefulness and Clinical Applications of 3D Printing in Cardiovascular Diseases 2.0
Topic Editors: Zhonghua Sun, Massimo Chessa, Israel Valverde, Alexander Van De BruaeneDeadline: 31 October 2023
Topic in
Biomolecules, Cells, Diseases, IJMS, JMP, Organoids, JCDD
Molecular and Cellular Mechanisms of Diseases: Heart Disease
Topic Editors: Klaus-Dieter Schlüter, Pasi Tavi, Ebru Arioglu-InanDeadline: 24 December 2023
Topic in
Diagnostics, Hearts, JCDD, JCM, JVD
Mechanical Circulatory Support in Heart Failure
Topic Editors: Anton Sabashnikov, Ilija DjordjevicDeadline: 31 December 2023
Topic in
Diagnostics, JCDD, JCM, JPM, Medicina
Cardiovascular Disease in 2023: Coronary Syndrome, Heart Failure and Structural Heart Disease
Topic Editors: Saverio Muscoli, Rafael Vidal-PerezDeadline: 31 January 2024

Conferences
Special Issues
Special Issue in
JCDD
New Pacing Techniques and Non-invasive Methods That May Improve Response and Patient Selection to Cardiac Resynchronization Therapy
Guest Editor: András VereckeiDeadline: 15 September 2023
Special Issue in
JCDD
Heart Failure: Clinical Diagnostics and Treatment
Guest Editors: Nicolas Merke, Daniel A. Morris, Evgeny BelyavskiyDeadline: 30 September 2023
Special Issue in
JCDD
Peripheral Artery Disease (PAD): Risk Factors, Diagnosis and Treatment
Guest Editor: Zoltán RuzsaDeadline: 15 October 2023
Special Issue in
JCDD
Electropathology as the Foundation of Innovation in Diagnosis and Therapy of Atrial Fibrillation
Guest Editors: Bianca Brundel, Natasja de GrootDeadline: 1 November 2023















